What Is Metaflammation?

Metaflammation is the chronic, low-grade inflammatory state that develops when cortisol remains elevated over time. It's one of the primary drivers of weight loss resistance and metabolic decline.
When cortisol stays high for months or years, it progressively disrupts insulin signaling. Your cells become less responsive to insulin's message to absorb and use blood glucose. This is insulin resistance. It slows fat oxidation, disrupts hormonal balance, reduces your body's ability to use fat for fuel while simultaneously promoting fat storage, and creates a feedback loop where the more inflamed your metabolism becomes, the harder it is to regulate energy properly.
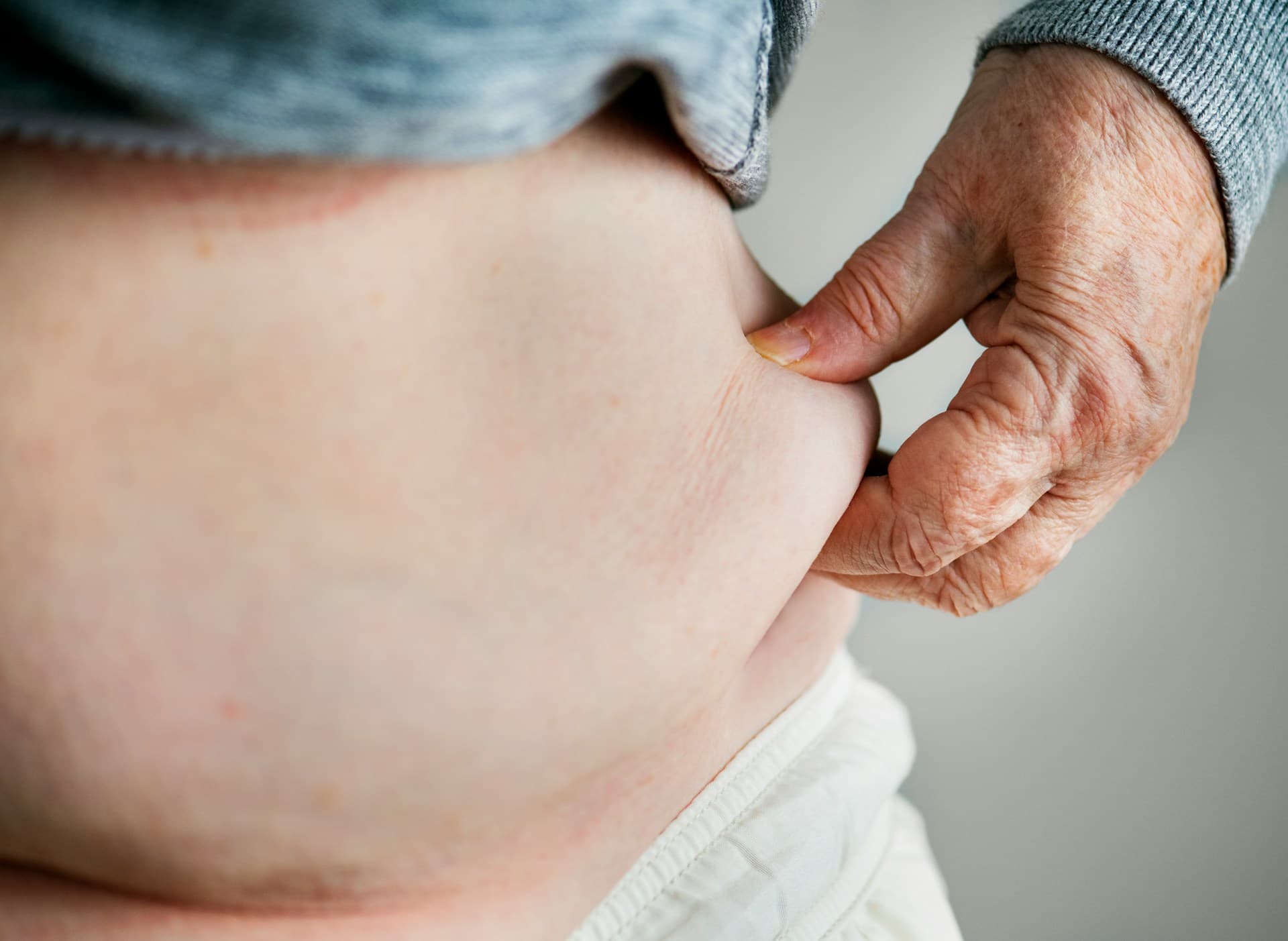
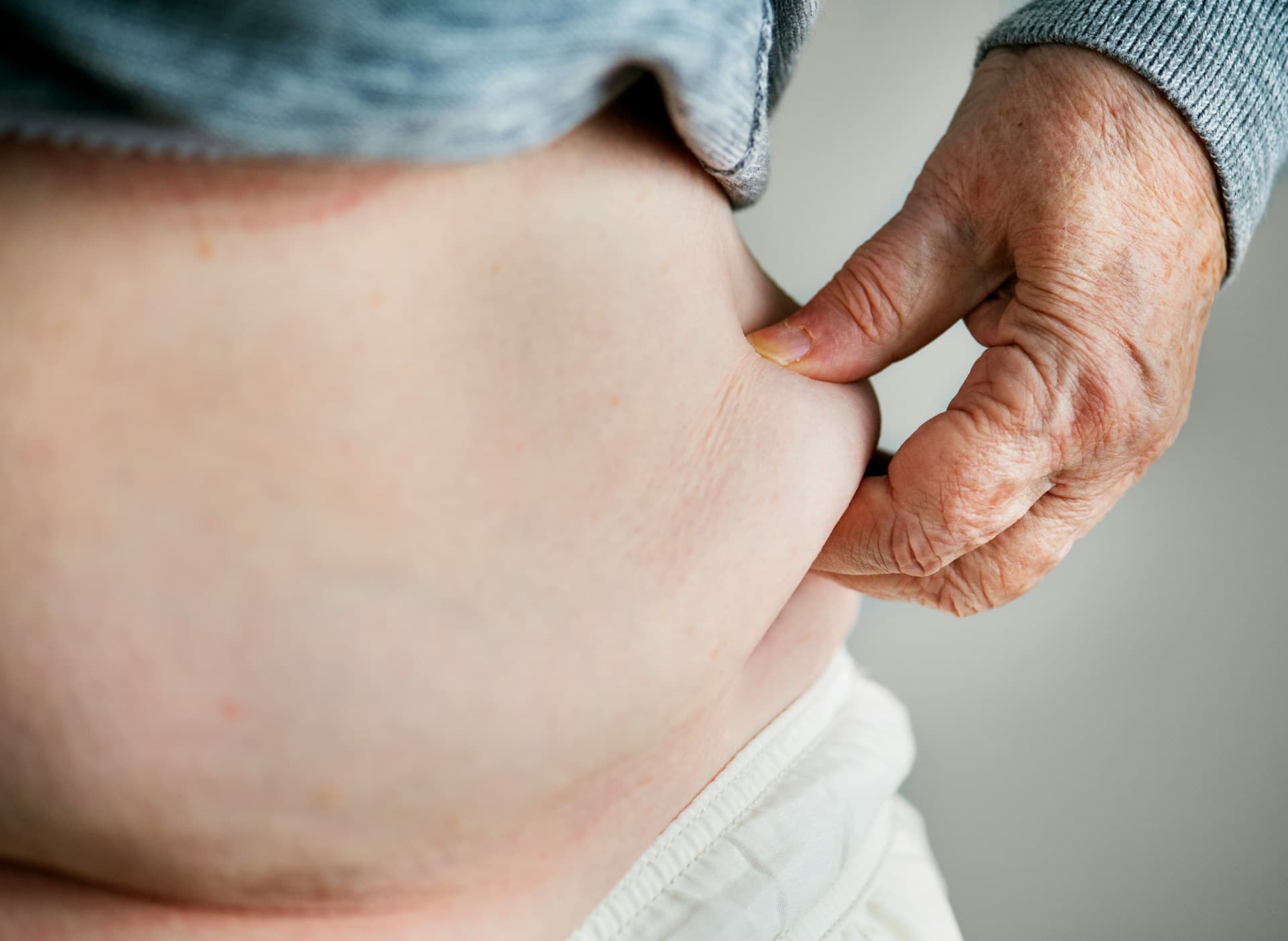
This is what we call metaflammation. It's the hidden driver behind midsection weight that doesn't respond to standard diet-and-exercise approaches. For a deeper look at why this is especially prevalent in middle age, read our post on why you can't lose weight in your 40s.