What Does Poor Sleep Actually Do to Your Metabolism?

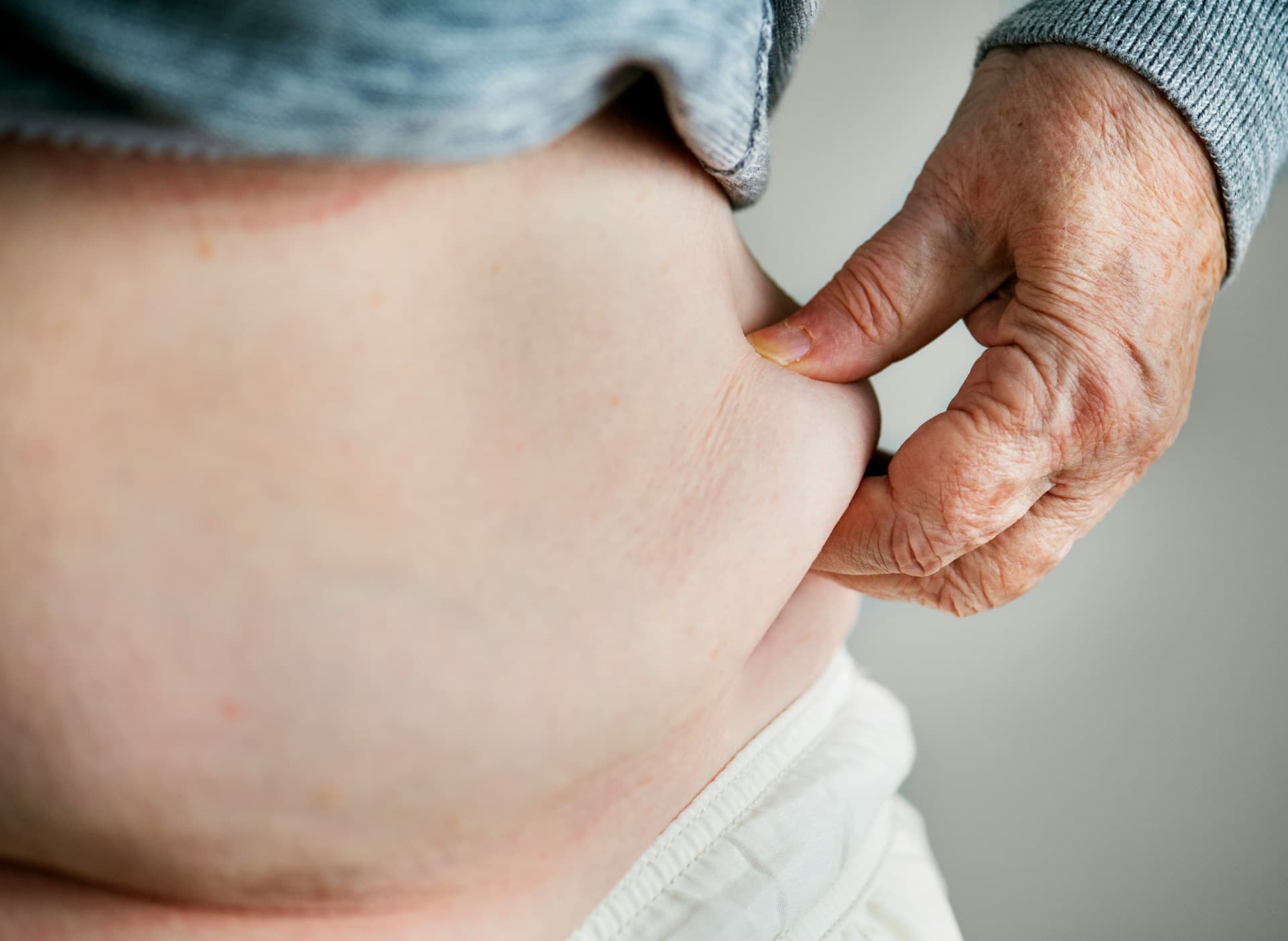
Sleep deprivation elevates cortisol, which drives blood sugar dysregulation, increases visceral fat storage, and suppresses the anabolic hormones like testosterone and growth hormone that your body needs to build and maintain lean mass.
The hormonal cascade from poor sleep is consistent: cortisol rises, leptin drops, ghrelin rises, and both growth hormone and testosterone are suppressed. Growth hormone and testosterone are primarily secreted during deep sleep. Poor sleep quality reduces both, accelerating the lean muscle loss that slows metabolism and makes weight management harder over time. For a deeper look at how testosterone decline compounds this picture in men, see our post on understanding low testosterone symptoms.