How Cortisol 'Steals' From Your Sex Hormones
Pregnenolone is the master precursor hormone from which your body produces both cortisol and sex hormones. Under chronic stress, your body prioritizes cortisol production, diverting pregnenolone away from estrogen and progesterone synthesis. This is known as the "pregnenolone steal."
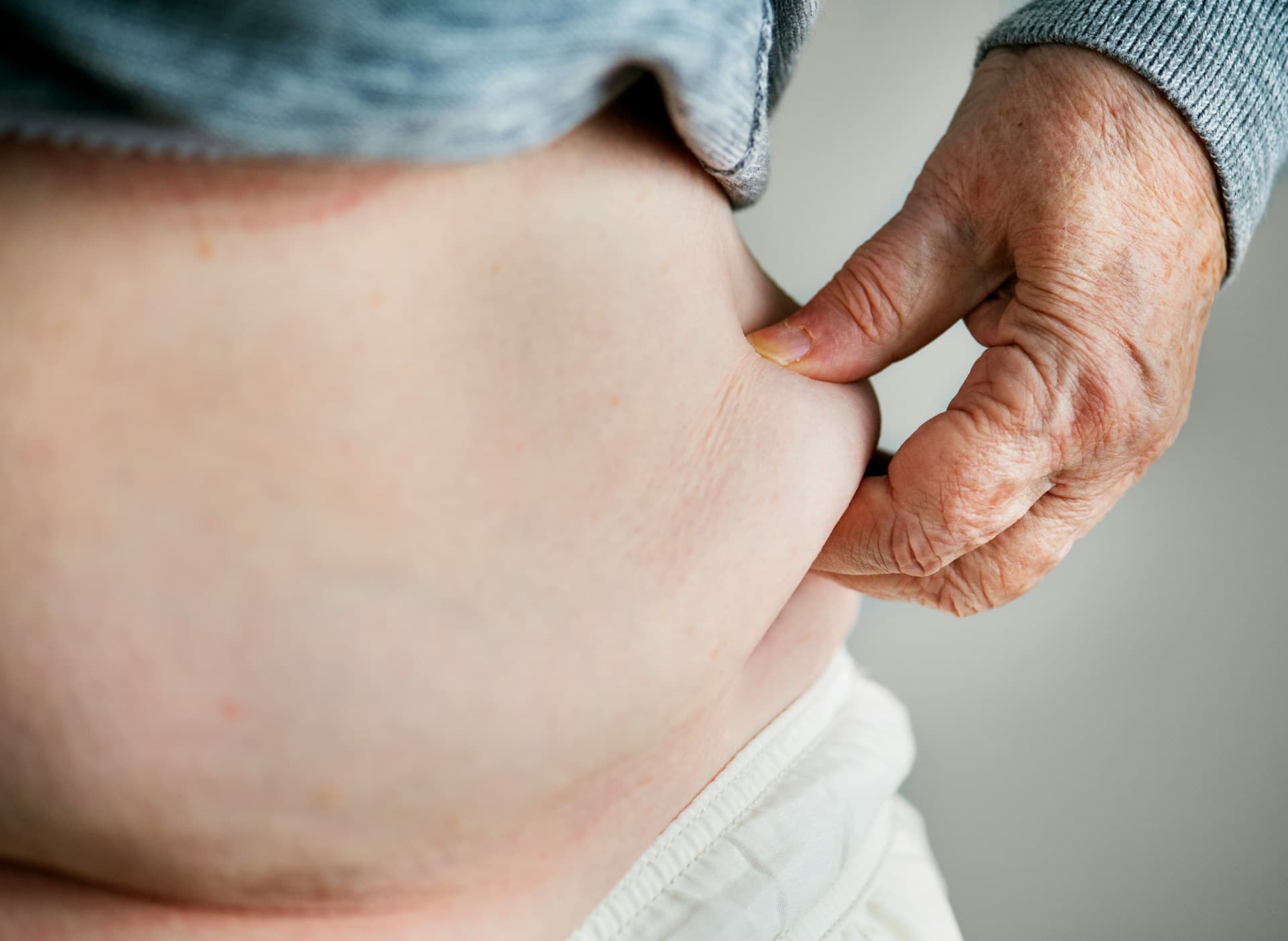
Progesterone is particularly vulnerable because it sits directly on the cortisol production pathway. When demand for cortisol is high, progesterone is literally consumed in the process of making it. This is why stressed women in perimenopause often experience progesterone-related symptoms (anxiety, insomnia, irregular cycles) before estrogen decline becomes pronounced.
For a deeper understanding of how estrogen and progesterone interact, see our post on estrogen vs. progesterone and hormone balance.