What Stress Actually Does to Your Metabolism

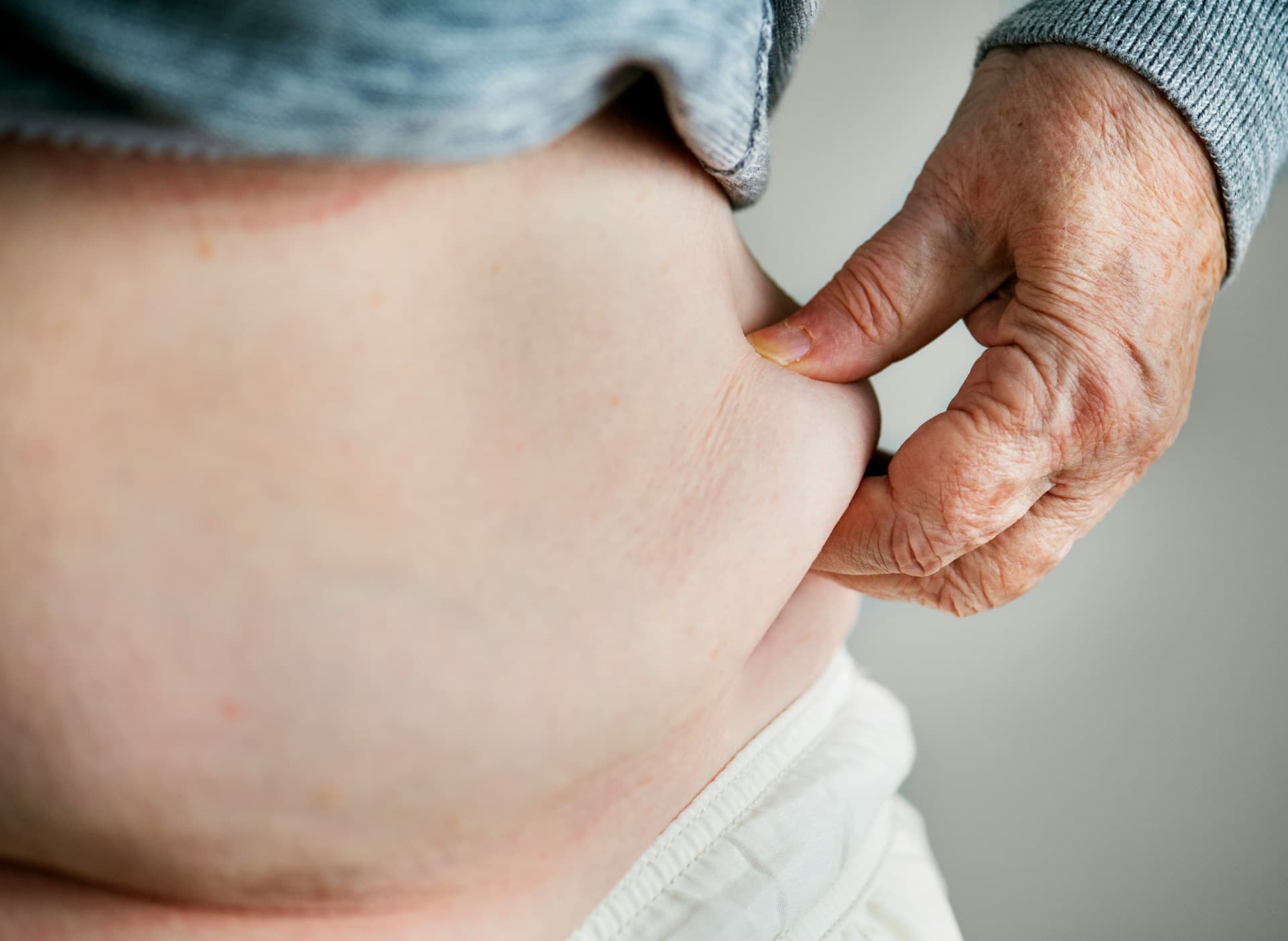
Cortisol signals the liver to release glucose into the bloodstream in preparation for a physical threat. When that threat is psychological and the glucose goes unused, it's stored as visceral fat around the abdomen and organs.
Your stress response was built for a world where stress meant physical danger. Sustained pressure from work, relationships, finances, and daily demands keeps cortisol elevated for months and years. The glucose your liver releases has nowhere to go. It gets stored. Repeatedly. In the same place.
Over time, chronic cortisol elevation disrupts the hormonal signals that regulate appetite, energy, and sleep. Cortisol suppresses testosterone. It interferes with thyroid function. It blunts the effectiveness of leptin. The result is a metabolic environment working against you on multiple fronts simultaneously.